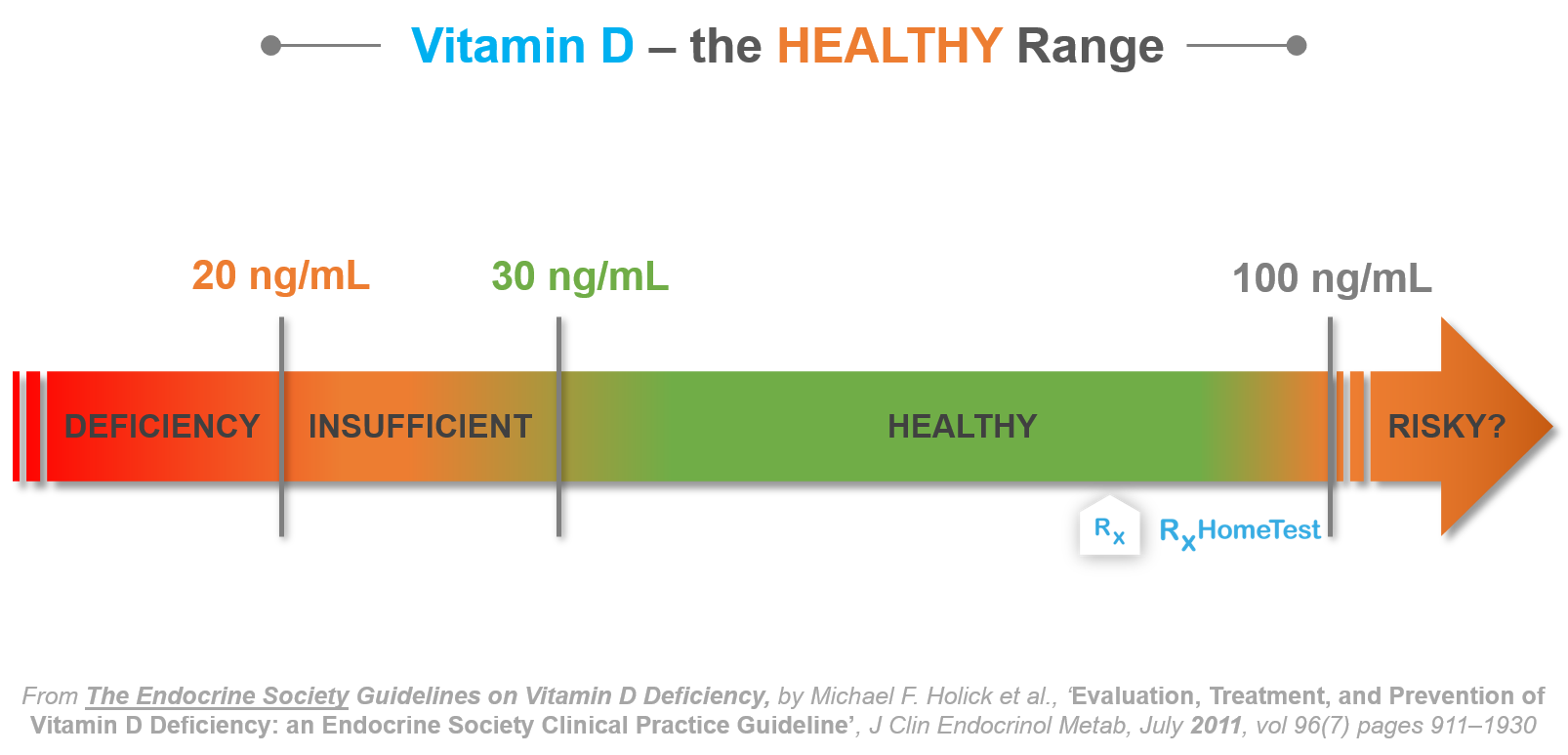
Vitamin D level ranges:
Deficient: below 20 ng/ml
Insufficient: 20-30 ng/ml
Normal Vitamin D level: > 30 ng/ml — recommended to maintain 30-40 ng/ml; your doctor will normally recommend to err on the higher side for both males and females.
Potential Overdose: 40-70 ng/ml
May be Toxic?: over 150 ng/ml — too much Vitamin D has potential risk of kidney stones and high calcium.
Note the units in ng/ml (1 ng/ml is equal to 2.5 nmol/l).
Reference: Evaluation, Treatment, and Prevention of Vitamin D Deficiency: an Endocrine Society Clinical Practice Guideline by Holick et. al. in The Journal of Clinical Endocrinology & Metabolism 96, 2011.
Vitamin D is very important for bone health because it helps in the absorption of calcium and phosphorus.
Research shows it has many uses, including in heart health and for fighting over 15 different types of cancers.
Despite plentiful sunlight, a large population has low Vitamin D as people tend to avoid direct exposure to sun.
Your doctor will most likely recommend maintaining normal Vitamin D levels of at least 20-30 ng/ml. But too much Vit D is rarely an issue, so general recommendation is to get more, if possible.
Vitamin D enriched foods or supplements are popular methods to make up for any deficiency. An easy and simple at-home Vitamin D test kit can help check your levels if you suspect a deficiency.
Most Vit D is stored in liver before it reach the blood through kidneys. Therefore, it's important to measure the normal Vitamin D3 levels, which is one of the type found in humans.
Too much Vitamin D can cause toxicity but it's rare. However, it might increase your risk of kidney stones.
Vitamins, by definition, are things that our body does NOT make on its own. But, Vitamin D is unique because of the way it is named (it's a hormone and that's why the confusion).
Then, how's it made? In short: by using sunlight and cholesterol.
With UVB rays in the sunlight (these are bluer-than-blue light, at wavelengths of 290-310 nm), our body converts skin cholesterol into a form that can be easily absorbed and stored.
This precursor to Vitamin D is stored in the liver—the way water is stored in a camel’s hump. Then it is released into the kidneys in the final active form that circulates in the blood.
Absorption of calcium and phosphorus depends on Vit D. These minerals are essential for maintaining healthy bones, especially in children and seniors. Insufficient levels can cause fractures and bone loss.
Our bodies have 26 Vitamin D responsive tissues that require adequate levels to activate their functions, which affect over 200 genes in the body.

READ MORE FROM OUR BLOGS:
The Most Common Signs of Vitamin D Deficiency – notice the early signs before supplementing.
The Best Ways To Manage Your Vitamin D Levels – quick & easy steps to follow.
The Benefits of At-Home Health Test Kits – how an at-home Vitamin D test might help.
Vitamin D and CVD – role of Vitamin D in heart health health.
An Easy, Simple Vitamin D Test – get tested with a few drops of blood collected at home.
Hormone Imbalance in Women – learn about the role of estrogen, progesterone and testosterone for women.
Despite abundant sunlight, a large population has low Vitamin D. That is because people proactively avoid exposure to sun. Vitamin D levels in females might even be lower as they often avoid sunlight due to cultural and aesthetic reasons.
Also, for almost 6 months a year, large parts of US and Canada don’t receive UVB rays that are necessary to make Vit D. In winter months, from November to March, these rays are blocked by the ozone layer.
That's why foods rich in Vitamin D such as milk, eggs, and supplements are popular to avoid any deficiency.
Doctors normally recommend maintaining levels of at least 20-30 nl/ml, although higher levels are often better. It's best to get tested before supplementing.
Too much Vitamin D and toxicity is extremely rare (can excess sunlight cause toxicity?) but those taking the supplements should monitor their levels regularly to avoid overconsuming. In extreme cases, very high levels may lead to kidney stones.
Vitamin D3 or cholecalciferol – this form is naturally produced by the body. It is rarely toxic, because higher levels (>20 kIU) are removed by the body. Cholecalciferol is the most common type available in supplements.
Vitamin D2 or ergocalciferol – this form is produced in plants and fungi but not in humans, therefore vegan Vitamin D. Prescription medications of Vit D2, e.g., for treating parathyroid are called calciferol. However, ergocalciferol is half as effective as Vit D3 and you may need to take twice of Vit D2 when replaced with Vit D3.
It is interesting to note that both forms are fat soluble. That's why being overweight & obese can lead to low Vit D as fat absorbs and prevents releasing them into the body.
Because of its role in absorption of calcium and phosphorus in the body, low Vitamin D can cause serious health issues. For example, in:
Children: Rickets (weak, improper formation of bones).
Adults: Osteomalacia (low bone density, unhealthy bone repair, maintenance due to improper Ca, P absorption).
At Any age: Crucial for preventing and reducing multiple cancers (including cancers of breast, lung, colon, prostate). Also, important for cardiovascular health, bone fracture & fall, diabetes, stress & fatigue, and other common diseases.
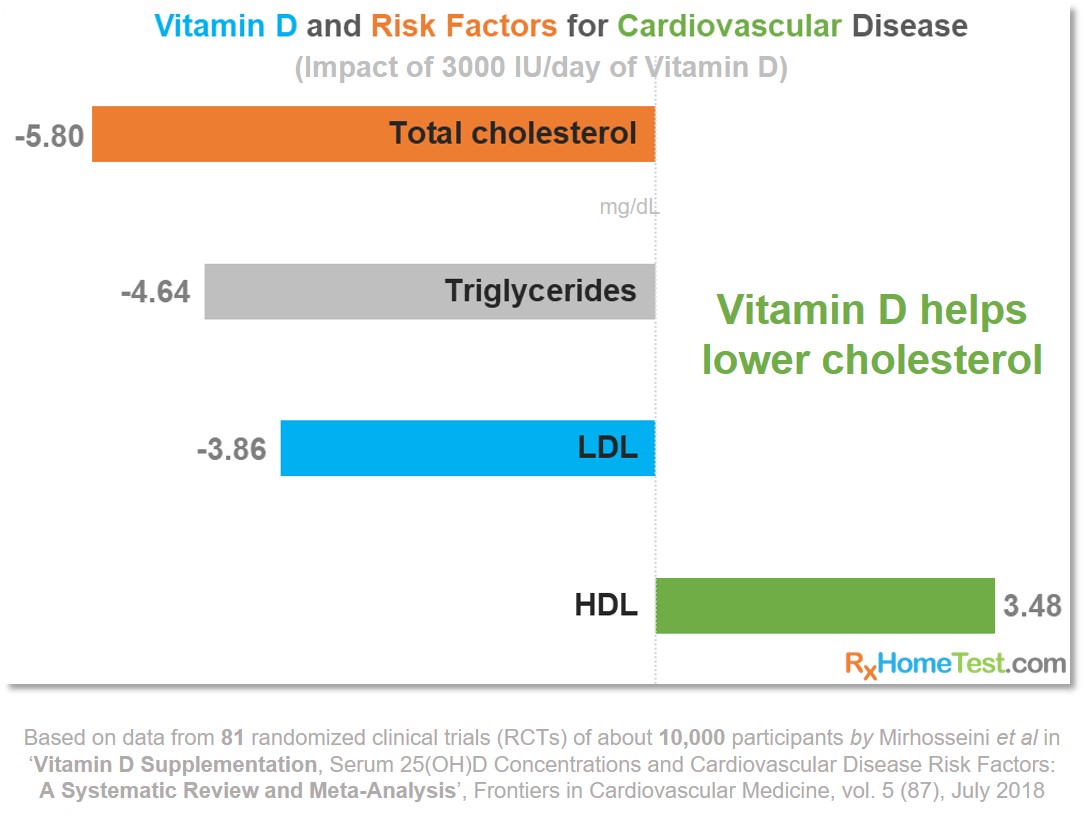
Source: Vitamin D Supplementation, Glycemic Control, and Insulin Resistance in Prediabetics: A Meta-Analysis by Mirhosseini et. al. in Journal of the Endocrine Society (2018).
There are four key steps that start with sunlight to the final production in our body:
First, exposure to sun (i.e., UVB rays) activates a type of cholesterol, 7-dehydrocholesterol (7-D) in the skin.
Then, 7-D becomes pre-Vitamin D & immediately becomes Vitamin D3.
Next, Vitamin D3 becomes 25-D in liver through hydroxylation and deposits in the liver (like a camel’s hump storing water).
Finally, the liver releases 25-D to kidneys where it becomes an active and potent form (1,25-D3). This form circulates in the body and maintains the amount of calcium. 1,25-D3 is the right form of Vitamin D to monitor as multiple cells and tissues have receptors to convert 25-D to 1,25-D3 making it critical in other parts of body.
Excess 25-D converts to 1,25-D3 in other cells and tissues besides kidneys.
1,25-D3 (i.e., Vitamin D3) is the right form of Vitamin D to monitor with a test.
Not all sunlight is the same:
UVB rays are main source that activate Vitamin D (it's a very narrow band at 290-315 nm wavelength; the range of visible light is 360 nm(violet) -780 nm(red)). However, it can’t penetrate very deep, even window glass will block it.
UVA rays (>315nm wavelength) penetrate deeper but do not prompt skin to make Vitamin D; cause wrinkles, aging, skin discoloration.
At organ and cellular levels, Vitamin D absorption goes through multiple steps:
Regular metabolism: From Liver (as 25-D) –> into bloodstream –> into kidneys (1,25-D3: active, vital form) –> into bloodstream –>finally into intestinal cells (absorption of Ca, P –> healthy bones).
Autocrine cell functions (metabolism in the tissues and cells, a role discovered based on research in past 20-25 years): from Liver (as 25-D) –> into most organs of the body with Vitamin D receptors (1,25 D3: active, vital form) –> finally utilized by cells & tissues (essential for preventing cancers & other diseases).

Source: Vitamin D Supplementation, Glycemic Control, and Insulin Resistance in Prediabetics: A Meta-Analysis by Mirhosseini et. al. in Journal of the Endocrine Society 2, 2018.
Reasons why people avoid sunlight:
Fear of skin-cancer
Aging
Wrinkled skin
Discoloration of skin
Common sources include
Sunlight – the best way to get Vitamin D (however, only UVB: 290nm – 315nm wavelength, deep violet, not visible to the eye)
Fish liver oil (cod-liver, salmon)
Supplements
Tanning beds
Fortified food (milk, orange juice, cereals, margarine, etc.)
Most food items don’t have Vitamin D or barely have any
From Sun: There is no maximum dose of Vitamin D. But standing in sun for 12 minutes at noon with bare arms & legs for a white woman will give roughly equal to 3000 IU. For 30 minutes, is equivalent to 20,000 IU. People with darker skin will need more since the melanin in skin will absorb some of the sun.
From Cod-liver: best natural food source at 1360 IU per tablespoon. However, one should watch out for excess Vitamin A in it which can be toxic!
Fortified food: 85% of winter supply comes from foods enriched in Vitamin D, depending on the country (as govt controls the foods that can be fortified). Fortified milk is one of the most popular foods high in calcium and Vitamin D.
In US: milk, cereals, orange juice, margarine.
In Canada: only milk and margarine.
Even fewer options for those who are lactose intolerant or vegetarian or vegan.
You may not always need to supplement. If you get enough sunlight, try to:
Find the time it takes for the skin to turn pink (depends on skin tone, time of day, season, etc.).
25-50% of this time will give 1,000 IU.
Try few times a week in summer to get sufficient dose of UVB and let it store in liver.
The CDC's recommended dose of Vitamin D of 200 IU per day seems outdated.
Recommended daily allowance (RDA) as per the CDC direction are:
50 years or younger: 200 IU per day.
Over 50 years: 400 IU per day.
Upper safe limit: 2000 IU/day** Most medical professional recommend 5-10 times higher dose and are asking government to revisit these limits setup in 1997 (note 30 minutes of full Sun exposure gives as much as 20,000 IU!!). Therefore, the maximum daily dose of Vitamin D as per CDC is really low.
A note on the units:
In food & other sources: IU (International Unit); 1000 IU = 25 microgram of Vitamin D (for other Vitamins, microgram/IU can be different). This is the unit you see on Vitamin D supplements. A 2,000 daily dose is basically 50 microgram.
When measured in the blood: ng/ml (1 ng/ml = 2.5 nmol/l). This is what you will see when tested using an at-home
The best way to get Vitamin D is sunlight. Sea foods are the most common natural sources of Vitamin D. But supplements are frequently used.
Most common sources with approximate amounts are:
Cod-liver oil: 1360 IU in 1 tablespoon
Salmon: 360 IU (3.5 oz, cooked)
Mackerel: 345 IU (3.5 oz, cooked)
Sardines: 250 IU (1.75 oz, canned in oil)
Tuna fish: 200 IU (3 oz, cooked)
Milk: 98 IU (fortified, 1 cup; you need 10 cups for 1,000 IU!!)
Margarine: 60 IU (1 tablespoon, fortified)
Egg: 20 IU (one egg with yolk)
Beef: 15 IU (3.5 oz)
Cheese: 12 IU (1 oz)
Tanning beds: helpful but are known to cause skin cancers & generally not recommended. Otherwise, the same exposure advise as for Sun: 25-25% of time it takes to turn your skin pink.
Multivitamins: Okay to use but note overdose of other vitamins can be toxic (e.g., too much Vitamin A is known to be toxic).
Latitude – i.e., how far from equator. Larger distance means UVB rays go through a longer ozone layer and get absorbed more. Beyond 35 degrees latitude north or south, almost no UVB reach the surface from Nov to March (regions north of Flagstaff AZ, Albuquerque NM, Knoxville TN, Oklahoma city OK, Charlotte NC). For reference, Canadian border is at 49th parallel and Portland OR is near 45th parallel.
Altitude – i.e., height above see level. Lower altitudes absorb more UVB and make less of it. People in mountains get more UVB.
Season of the year – Winter months get less sun.
Time of the day – need UV Index of 3 or more; 10 am – 2 pm are best times.
Air pollution – particles absorb UVB and reduce the production.
Cloud cover blocks the sun; the US Pacific Northwest region with long rainy periods will get less sun and thus lower production in skin.
People with darker skin may need more sunlight for healthy Vitamin D levels, as melanin in skin absorbs the sunlight.
Sunscreen or sunblock – absorb the sunlight and hence prevent the body in making it. Higher SPF means higher sun block (e.g., SPF8 blocks 92% skin’s production; SPF15 blocks 99%). General advise is to soak in sun for few minutes before applying sunscreen.
Melanin – darker skin has higher melanin which absorbs more sunlight and competes with Vitamin D production; people from Africa need almost 10 times more UVB exposure.
Age – those at older age have less 7-D in the skin and need almost 25-50% more sunlight.
Weight – Vitamin D is fat soluble thus fat cells in skin will dissolve making less of it available for tissues and organs.
Clothing – body coverage blocks the sunlight, e.g., Islamic women & men as well as people in cold places with more body coverage will get less sun exposure.
There are other subtle factors that may play a role:
People often consider deficiency as a new fad.
Several important roles of Vitamin D are discovered only recently in past few decades.
Awareness of skin cancer from sunlight is much higher.
Perception that inadequate sun exposure only impacts childhood growth.
Symptoms are subtle and easy to confuse with other medical conditions, e.g., with food sensitivity to something in diet.
Symptoms of low Vitamin D levels are subtle and can be easily confused with other health conditions.
Muscular weakness (weak muscles)
Feeling of heaviness in the legs
Chronic musculoskeletal pain (chronic pain in muscles and bones)
Fatigue or easy tiring
Frequent infections
Depression
Chronic pains, e.g., back pain, neck pain (defect in bone-hardening with deep, gnawing pain in muscles and bones)
Low levels in children: due to reduced outdoor activities and sunscreen protection.
Pregnant and nursing mothers: due to sharing with baby.
Obese and overweight: Vitamin D dissolves in fat and therefore fat cells can absorb and store, making less of it available.
Seniors: less Vitamin D precursor in skin (may need up to 4x Sun otherwise can result in weaker bones and fractures).
Others: People with Crohn’s disease, cystic fibrosis, gastric-bypass surgery, liver or kidney failure might not be able to absorb fat soluble Vitamin D.
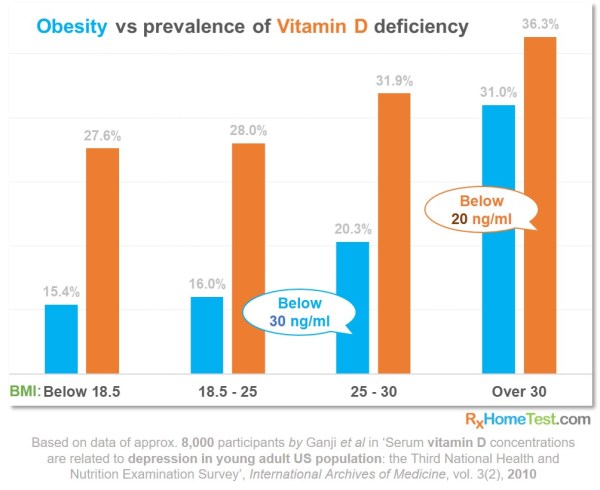
Despite all the awareness, a significant part of the population is deficient. Without getting tested, it is very difficult to tell the levels. Those working indoors do not get enough exposure to sun and end up being deficient.
Symptoms are subtle and can be confused with other medical conditions.
It has been shown to play a key role in fighting over 15 different kinds of cancers and new research suggests it is important for other key roles and not just for bone health.
Those with darker skin need even more sun since the melanin in skin competes for sunlight. People from Africa, South East Asia, Latin and South America tend to believe deficiency is a problem only for people with fair skin. However, their darker skin color has naturally evolved for high sun exposure and when they live in regions farther away from equator their requirement for sun exposure increases as these regions get less sunlight.
During winter, when the sun is not directly above us, sunlight travels a longer path through the atmosphere. Therefore, more of the UVB rays are absorbed by the ozone layer and the remaining sunlight can not produce as much on exposure to skin. In fact, regions north of 35th parallel (north of Phoenix, Bakersfield, Albuquerque, Knoxville, Oklahoma City, Charlotte, Raleigh) get almost no UVB from Nov to Mar.
Glass windows, sunscreens block the Vitamin D producing part of the sunlight, filtered light produces almost none of it.
Children need calcium and phosphorus for developing their bones require it as key ingredient in absorbing the minerals.
Bone density decreases with age, which requires higher levels for maintaining healthy bones.
Vitamin D has been shown to reduce fractures among elderly.
As fat cells dissolves it, obese and overweight people need more to compensate.
Few naturally occurring food items contain Vitamin D. Vegetarian and vegan diets make the choices extremely limited.
It is always a good idea to test your Vitamin D levels before taking supplements or increasing your doses.
The most popular test for Vitamin D is using a simple finger prick blood sample. You can order an that can accurately measure the active form of Vitamin D (1,25-D3) in blood stream. The kit can be ordered online & a blood sample can be provided from home without the need to visit a doctor or any labs. The comprehensive lab report will clearly explain your results.
More comprehensive but expensive test is LC-MS/MS (liquid chromatography tandem mass spectroscopy).
What's the Best Time to get tested?
* November: onset of Vitamin D winter (fall)
* March: end of winter (spring)

Source: Evaluation, Treatment, and Prevention of Vitamin D Deficiency: an Endocrine Society Clinical Practice Guideline by Holick et. al. in The Journal of Clinical Endocrinology & Metabolism, Vol 96 (7), 2011, Pages 1911–1930.
What physicians normally suggest (although one should confirm with a doctor before starting any of these regimens):
A 1,000 IU daily dose will increase levels in blood by 10 ng/ml in 3-4 months
If levels < 20 ng/ml, then 50 kIU/week for 8 weeks –> then may change to 2,000 IU per day
And if levels are 20-30 ng/ml: same as < 20 ng/ml
Otherwise, if levels are 30-40 ng/ml: 50 kIU/week for 6 weeks –> then may change to 2,000 IU per day
Unborn babies: pre-natal vitamins have 400 IU
Breast feeding babies: 400 IU/day (nursing mothers need > 40 ng/ml and may need up to 4,000 IU/day)
Younger than 1 year: 400 IU/day
1-2 year old: 1,000-2,000 IU/day (based on weight
Over 12 years old: 2,000 IU/day
Excess Sun or skin based overdose is naturally protected by the body.
Overdose toxicity of 150 ng/ml can only be achieved by several months of >10,000 IU/day. It is very hard to get this level of overdose.
In reported literature, very few cases of overdose are reported. One case with 150,000 IU/day taken over two years resulted in 500 ng/ml but didn’t have any immediate health conditions after stopping.
Overdose (>150 ng/ml) may result in elevated calcium in blood that can cause:
Abdominal pain
Constipation
Muscle weakness
Itching
Vomiting
Extreme thirst
Predisposition to kidney stones and high blood pressure
Vitamin D raises calcium levels which may increase the risk of kidney stones.
Also, high levels are not for:
Those with Lymphomas should avoid supplementing it.
People with granulomatous diseases (Tuberculosis and Sarcoidosis) – keep 20-30 ng/ml.
Drugs that lower the levels (drugs for seizures; cimetidine, steroids, certain asthma medicines, and weight loss drugs).
Anyone taking the drug hydrochlorothiazide (mild diuretic) for high blood pressure should not supplement as this.
Source: Vitamin D Revolution by Soram Khalsa, M. D.
For more information & references, visit the NIH page on Vitamin D.